Navitus releases Drug Trend Report, “Clarity for Action”
Navitus releases Drug Trend Report, “Clarity for Action”
New analysis explains rising prescription costs and actions to counter national trends
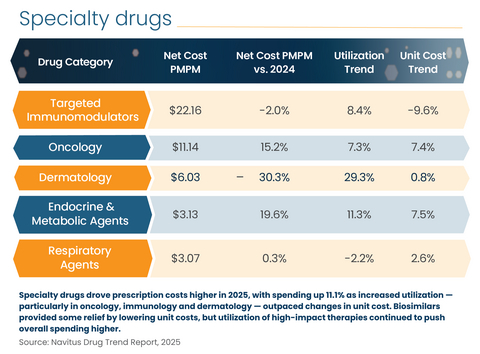
Specialty drugs drove prescription costs higher in 2025, with spending up 11.1% as increased utilization — particularly in oncology, immunology and dermatology — outpaced changes in unit cost. Biosimilars provided some relief by lowering unit costs, but utilization of high-impact therapies continued to push overall spending higher.
MADISON, Wis.--(BUSINESS WIRE)--Navitus today released its 10th annual Drug Trend Report, “Clarity for Action,” the company’s flagship annual analysis of prescription drug cost trends. The report details how utilization growth and therapeutic innovation drove prescription drug costs in 2025 and outlines clear actions for health plans and plan sponsors to counter accelerating pressure.
Across the Navitus commercial book of business, net prescription drug costs increased 8.4%, up from 7% in 2024, largely reflecting demand for high‑cost specialty medications. Despite industry pressures, Navitus enabled 32% of clients to pay less in 2025 than in 2024, and 44% to limit increases to no more than 5%. The Navitus trend also remained below double-digit increases seen in the industry.
“Drug trend is no longer driven primarily by price inflation. It’s also being driven by increased utilization and expanded indications,” said Sharon Faust, Navitus Senior Vice President and Chief Pharmacy Officer. “Existing therapies with broader indications are gaining earlier adoption. These advances demand deliberate, informed management to ensure that costs remain sustainable.”
Specialty and non‑specialty trends shape drug trend
Specialty medications remained the largest driver of drug costs in 2025, with an 11.1% increase. Growth came from increased utilization, particularly in oncology, immunology and dermatology. Biosimilars provided relief by lowering unit costs, but utilization of high‑impact therapies continued to exert upward pressure.
Non‑specialty drug costs increased 5.6%, reflecting rising utilization and steady unit‑cost growth. Diabetes therapies, especially GLP‑1 medications, played a major role, with Mounjaro representing the single largest cost-growth medication. Without GLP-1s, the overall Navitus drug trend was 7.9%. Migraine treatments added trend pressure as well. These increases were partially offset by generic drug launches and reduced utilization in ADHD, cardiovascular and antiviral medications.
“What stands out is how quickly utilization patterns are changing,” Faust said. “Members and prescribers are moving rapidly toward newer and more effective therapies. That shift is happening across nearly every major category.”
Looking ahead: Trend pressures expected to intensify
Drug trend is expected to accelerate in 2026 and beyond, with new biologics and targeted therapies entering the market at premium prices. Utilization is also expected to climb as therapies gain earlier and expanded use. In non‑specialty categories, GLP‑1 medications are expected to remain a dominant cost driver, supported by broader prescriber adoption and patient demand. Migraine care also is expected to continue shifting toward higher‑cost brand-name medications.
What health plans and plan sponsors can do
The report emphasizes that rising drug trend is not inevitable or uncontrollable, but it does require early, informed action. Navitus experts identify proven strategies for managing trend, including:
- Adopting generics and biosimilars, particularly in high‑cost specialty categories, which saved Navitus clients $56 million in one treatment category alone in 2025
- Using evidence‑based formularies prioritizing lowest net cost and clinical integrity
- Applying disciplined utilization management, ensuring proper therapy selection
- Demanding transparent reporting and pass‑through pricing to clearly understand true drug costs, following Navitus’ industry-leading model
“Plans have more control than they often realize,” Faust said. “The key is clarity to know what’s driving trend early and having a pharmacy solutions partner that acts quickly with disciplined, evidence‑based options.”
To access the full report, visit: https://navitus.com/drug-trend-reports/2025-drug-trend-report/?utm_campaign=100247_2025_drug_trend_report_dtr&utm_medium=press_release&utm_source=businesswire
“This report is about understanding what forces are driving costs and what actions make a difference,” Faust said. “As drug trend accelerates, plans and plan sponsors need insight they can trust and strategies they can deploy in time to matter.”
About Navitus
Navitus remains the nation’s first transparent, pass-through pharmacy benefit manager (PBM), serving more than 13 million lives nationwide. It uniquely brings clarity to drug pricing and takes costs out of the drug supply chain. Unlike traditional PBMs that generate profit by retaining an undisclosed portion of rebates and discounts negotiated with drug manufacturers and pharmacies, Navitus passes along the complete savings to clients, enabling them to make medication more affordable for their members. The Navitus PBM was established more than 20 years ago by Navitus Health Solutions, LLC, a pioneering pharmacy solutions company. The organization delivers a range of services through portfolio brands including Navitus, Lumicera, Archimedes and Clarventa. Owned by SSM Health and Costco, Navitus Health Solutions serves nearly 20 million lives across 800 clients including employers, unions, government plans, payers and health systems.
Contacts
For questions and media inquiries
Please email navitus@aircoverpr.com