UnitedHealthcare Introduces AI Companion Empowering People with Simpler Navigation, Personal Experience
UnitedHealthcare Introduces AI Companion Empowering People with Simpler Navigation, Personal Experience
- Avery responds in natural language 24/7 with personal coverage and claims details, cost estimates, scheduling help, care options, rewards opportunities and more
- Avery offers customer advocates real-time insights into member experience, case history
- Avery helps guide members to more affordable quality care, potential savings
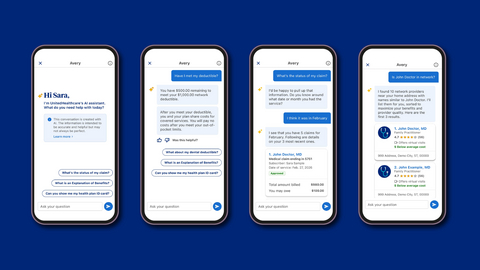
--(BUSINESS WIRE)--UnitedHealthcare today introduced Avery, a generative AI companion that creates a simpler, more coordinated health care experience for members while empowering customer advocates to more efficiently respond to members.
“People want health care to be easier to use and tailored to their personal needs,” said Dan Kueter, CEO for UnitedHealthcare’s commercial business.
Share
Available to eligible members through the UnitedHealthcare® app or myuhc.com®, Avery learns from people’s interactions with it and provides powerful self-serve capabilities. Avery adapts to the user, offering a more personalized experience based on the individual’s specific benefits and demographics. Avery offers clear, actionable next steps for members and advocates in real-time.
“People want health care to be easier to use and tailored to their personal needs,” said Dan Kueter, CEO for UnitedHealthcare’s commercial business. “Avery is one way we are responding to consumer demand for a more coordinated and simpler experience and enabling our members to focus on what matters most: getting and staying well.”
Avery is currently available to approximately 6.5 million members with UnitedHealthcare employer-sponsored health plans and 160,000 Medicare Advantage members, with expansion to reach a total of 20.5 million commercial, Medicare and Medicaid members by the end of the year.
Avery can help members with a wide range of questions and issues related to: coverage and personal benefits; appointment scheduling; cost estimates and plan balances; rewards opportunities and wellness programs; ID cards and over-the-counter benefits; provider search; claim approval status; and explanations of benefits.
UnitedHealthcare’s AI tools like Avery operate within rigorous oversight and governance frameworks designed to ensure safety, fairness and privacy with human expertise guiding output.
Avery empowers customer advocates with real-time insights
While 90% of the time, members who use Avery have not required assistance from an advocate, Avery will automatically transfer members to advocates when a live call is needed or requested. Avery provides a full synopsis to advocates if deeper support is necessary, so members do not need to repeat themselves or re-upload documents.
For members with more complex needs or questions, Avery provides real‑time administrative support and insights into the member’s history and experience for advocates. Such continuity and support are unique to UnitedHealthcare’s integrated service model.
Advocates can rely on Avery to help resolve administrative issues for members faster and more efficiently through real-time, conversational support and guidance. With Avery, advocates can spend less time taking notes or searching for information, for example, and more time focused on the member.
Avery simplifies navigation
Avery brings together information from multiple sources about benefits, providers and claims into one simple, unified experience, so members spend less time searching for answers or toggling between digital tools and more time focused on their health.
Designed to support the entire care journey, Avery can call network primary care providers to schedule appointments on a member’s behalf, striving to reduce friction and administrative burden.
Avery is designed to understand members’ personal health benefits, and helps members more easily understand their coverage details, care options and costs before scheduling an appointment. Avery can help members maximize their benefits, more easily find network providers and compare care options based on costs and their personal preferences.
Avery helps guide members to quality, affordable network providers, and aligns with their benefits by utilizing UnitedHealthcare's provider search capability. Avery offers more transparency and supports more informed decision-making by helping members understand their cost and care options in advance.
Avery will continue to evolve to include new and more powerful functionality and best-in-class features.
Health care that works better for people
UnitedHealthcare is working to improve health care and address pain points in the health system to make care more consumer-friendly.
Using insights from billions of digital transactions, Avery is the latest of more than 1,000 AI solutions across UnitedHealth Group, the parent company of UnitedHealthcare. UnitedHealth Group plans to invest $1.6 billion in AI this year.
Learn more about UnitedHealthcare’s commitment to make health care work better for everyone.
About UnitedHealthcare
UnitedHealthcare is dedicated to helping people live healthier lives and making the health system work better for everyone by simplifying the health care experience, meeting consumer health and wellness needs, and sustaining trusted relationships with care providers. The company offers the full spectrum of health benefit programs for individuals, employers, and Medicare and Medicaid beneficiaries, and contracts directly with physicians, care professionals, hospitals and other care facilities. UnitedHealthcare is one of the businesses of UnitedHealth Group (NYSE: UNH), a diversified health care company. For more information, visit UnitedHealthcare at www.uhc.com or follow UnitedHealthcare on LinkedIn.